Have you ever found yourself scrolling through the internet to compare your symptoms to an online description? If you have, you’re not alone—in fact, WebMD generated nearly 80 million views in the month of June alone. However, when it comes to carpal tunnel, it’s best to have a qualified medical professional take a look at your wrist to provide an official diagnosis.
In this article, we break down some of the ways examiners will diagnose carpal tunnel so you know what you expect when you head into the doctor’s office.
Carpal Tunnel Diagnosis Tests
1. Phalen’s Maneuver: Sometimes referred to as the wrist-flexion test, this simple procedure requires that the patient place the backs of their hands together with their fingers pointing down. They will stay with their wrists flexed in this way for several minutes. If their fingertips go numb, they likely have carpal tunnel syndrome.
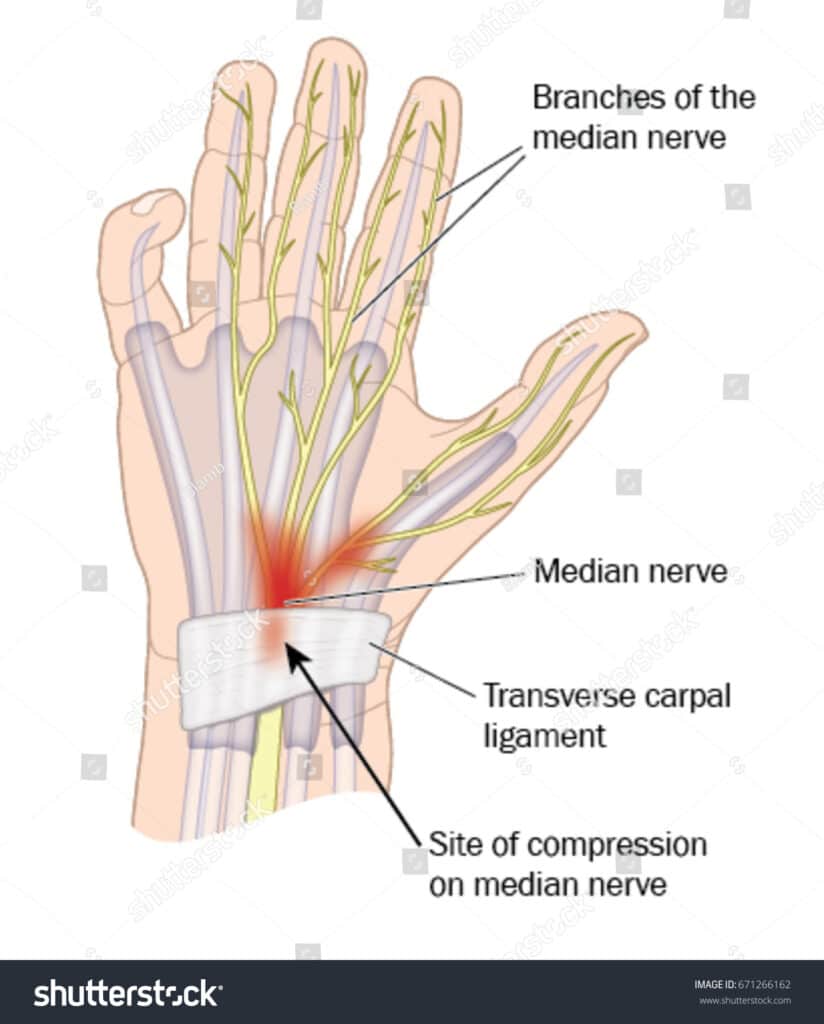
2. Tinel’s Sign: This is a common, non-invasive procedure for testing for carpal tunnel. During this test, the doctor will simply tap on the median nerve (located where the hand meets the forearm) with their finger or a reflex hammer. The patient with carpal tunnel will feel a pulse shoot up through their fingers like an electric shock. This may be as subtle as tingling in the fingertips.
3. Two-Point Discrimination Test: The name of this test refers to the patient’s ability (or inability) to discern a space between two points touching their arm from one. In this procedure, the doctor will likely use a two-point disc-criminator multiple times on each finger. (The two-point disc-criminator is a flat, octagonal-shaped instrument with needle-like protrusions on every side.) During this test, the doctor will start with the points of pressure a few centimeters apart and gradually move them closer until the patient can only discern one point of contact. This gives the doctor more specific information on the state of the compressed nerves—useful for carpal tunnel patients.
4. Electromyogram: In this slightly more invasive procedure, the doctor uses a needle to send electric currents from the muscles in the patient’s hand to their median nerve. The patient will flex their hand multiple times so the doctor can determine if the median nerve is compressed. This procedure should not be terribly painful—once the needles are removed, any discomfort should cease.
5. Nerve Conduction Velocity Test: Simply put, this test measures the speed at which a nerve can transmit an electrical signal. Like with the electromyogram, the doctor relies on electrodes to transmit an electric signal. In this procedure, the doctor places an electrode near your elbow and sends a current down through your median nerve. The longer it takes the current to reach the patient’s fingertips, the more compressed or damaged their median nerve.
Summary
While all of the above tests will let a doctor know if a patient is likely to have carpal tunnel, they may also choose to perform an x-ray, MRI, or ultrasound to rule out a diagnosis like arthritis. Knowing more about the patient’s daily habits, age, and overall health help a doctor decide which test to perform first to confirm or rule out carpal tunnel.
If you’re interested in being seen by a carpal tunnel specialist in the Salt Lake City area, click the link to learn more!
